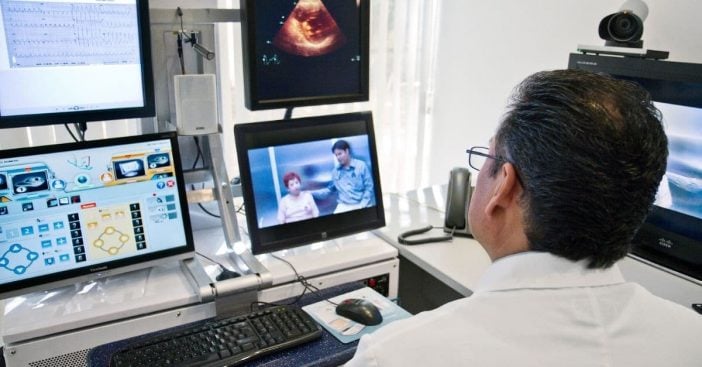
Even predicable events like doctor appointments can change, take on new forms. In the past, that always meant a house call, the special break in procedure to ensure quality healthcare continues within a person’s very own home. With time and technological advances, however, there’s a new special brand of healthcare replacing it: telemedicine.
This new form of medicinal delivery shows no signs of leaving, either, even before the pandemic. Over time, it manifested as remote access to healthcare providers via call and video. It also encourages doctors to quickly and remotely access health records from shared patients. Both in-person and digital approaches have their advantages and disadvantages, yet one is definitely gaining momentum.
Doctors, hospitals, and house calls, oh my

Since healthcare rose as a field centuries upon centuries ago, practitioners went to their patients to speak with them and observe their symptoms firsthand. When possible, patients also went to where their doctor practiced. Starting in the 1930s house calls enjoyed particular fame, making up about 40% of doctor-patient meetings. That’s almost half of all doctor-patient interactions occurring at home exclusively.
RELATED: Patch Adams: Robin Williams And The Real-Life Doctor He Portrayed
Remarkably, that number actually dropped exponentially leading up to the 1980s even before the big boom in telemedicine as we know it. Reasons include time efficiency and technological needs. Additionally, more specialists arose; these experts in their niche field could address problems primary care physicians might not have been able to. But house calls didn’t go away completely yet. In fact, its decline actually sparked a rise in team home care, which emphasizes a network based primarily at home to immediately meet a patient’s needs, especially if they’re older or very ill.
Telemedicine becomes a digital house call
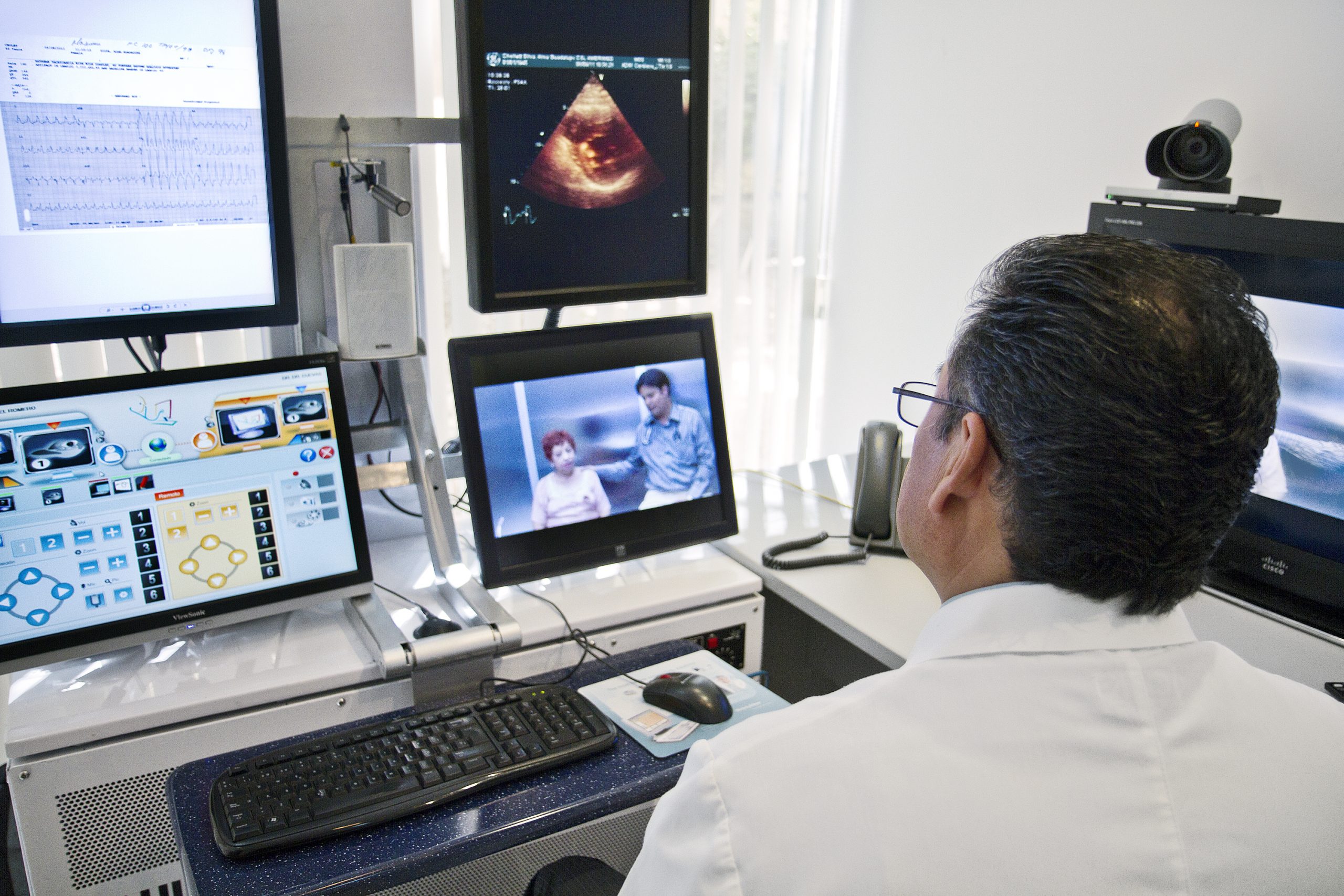
For the longest time, only healthcare providers had the physical tools (in additional to knowledge) to take important measurements to get a read on a person’s health. So, that meant they had to make a house call and take those measurements themselves with their tools. Now, however, technology has exponentially enabled telemedicine. A person can read their own blood pressure on a whim with a piece of Velcro around their wrist. Sleep studies require a microchip in their CPAP machines. They don’t have to go anywhere still, and neither does a doctor to get these numbers.
Instead, they remotely convey them to their primary physician or the specialist. That person can then also share it with other healthcare providers who may need to see it – with permission, of course. Telemedicine redefines the house call as calling a patient’s house via phone or video. By phone, this method appeared several decades ago, but now full-blown appointments can occur virtually.
A lot had to occur virtually in 2020, so with that increased use it saw this year, telemedicine shows no signs of dying down. In fact, MedCity News projects insurances will need to adjust their policies to account for an increased demand in telemedicine coverage. That just adds to the reduced travel costs for patients and some reduced costs for special tests. It won’t yet be able to replace everything and everything digital does come with privacy concerns. To best utilize this popular tool, everyone involved will need to think clearly and thoroughly about keeping it safe and convenient for all. If telemedicine becomes the new house call, hopefully it maximizes its benefits and eliminates its limits.
